LIVING LIFE WITH LUPUS

By: Meline Ngo
I’m 44 years old, and I am living with lupus for almost 20 years now. Well, first, what is lupus? This is the easiest way that I could explain what lupus is:
Lupus is a chronic autoimmune inflammatory disease that occurs when your body’s immune system attacks your own tissues and organs. It attacks healthy cells and tissues.
Autoimmune means your immune system cannot tell the difference between these foreign invaders and your body’s healthy tissues (“auto” means “self”) and creates autoantibody that attacks and destroys healthy tissue.
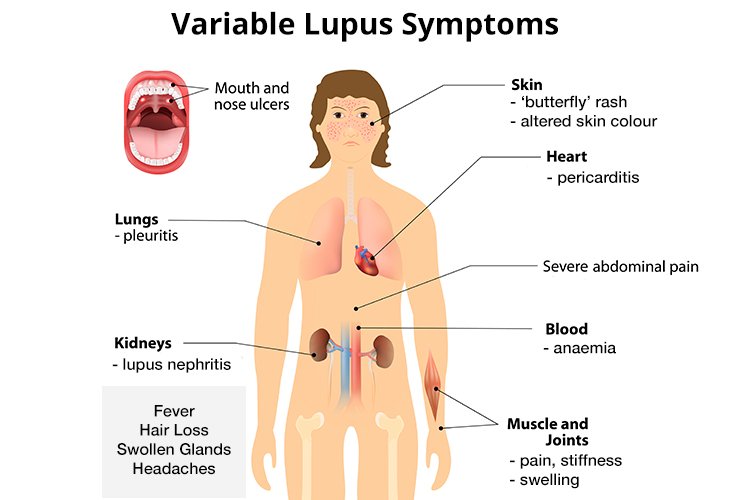
These autoantibodies cause inflammation, pain, and damage in various parts of the body. Lupus can be difficult to diagnose because its signs and symptoms often mimic those of other ailments. This can damage many parts of the body, such as the Joint, Skin, Kidneys, Heart, Lungs, Blood vessels, and Brain.
[lupus_systemic] Lupus is a disease that can lead to inflammation in not just the joints and skin but also many other organs. These include the kidneys, the tissue lining the lungs (pleura) and the heart (pericardium), and the brain.
Anyone can get lupus. Lupus affects about 5 in 10,000 people. It appears that people with an inherited predisposition for lupus may develop the disease when they come into contact with something in the environment that can trigger lupus. The cause for lupus in most cases, however, is unknown. Some potential triggers include: Sunlight, Exposure to the sun may bring on lupus skin lesions or trigger an internal response in susceptible people. Infections: Having an infection can initiate lupus or cause a relapse in some people.
Medications, Lupus can be triggered by certain types of anti-seizure medications, blood pressure medications, and antibiotics. People who have drug-induced lupus usually see their symptoms go away when they stop taking the medication. Your sex affects 10 times as many women as men. Age. Although lupus occurs in people of all ages, it is most commonly diagnosed between 15 and 40.
No two cases of lupus are exactly alike. Signs and symptoms may come on suddenly or develop slowly, mild or severe, and may be temporary or permanent. Symptoms of lupus vary, but some of the most common symptoms of lupus are Pain or swelling in joints, Muscle pain, Fever with no known cause, Red rashes, most often on the face, Chest pain when taking a deep breath, Hair loss, Pale or purple fingers or toes, Sensitivity to the sun, Swelling in legs or around eyes, Mouth ulcers, Swollen glands, Feeling very tired. Less common symptoms include anemia (a decrease in red blood cells, Headaches, Dizzy spells, Feeling sad, Confusion, Seizures. Symptoms may come and go.
When a person is having symptoms, they are called flares, ranging from mild to severe. New symptoms may appear at any time. You may need special kinds of doctors to treat the many symptoms of lupus. While there’s no cure for lupus, treatments can help control symptoms. Your health care team may include Rheumatologists – doctors who treat arthritis and other diseases that cause swelling in the joints; Clinical immunologists – doctors who treat immune system disorders; Nephrologists – doctors who treat kidney disease; hematologists – doctors who treat blood disorders; Dermatologists – doctors who treat skin diseases; Neurologists – doctors who treat problems with the nervous system; Cardiologists – doctors who treat heart and blood vessel problems; Endocrinologists – doctors who treat problems related to the glands and hormones; Nurses, Psychologists.

The doctors develop a treatment plan to fit your needs. You and your doctor should review the plan often to be sure it is working. You should report new symptoms to your doctor right away so that treatment obtainable changed if needed. The treatment plan goals are to prevent flares, Treat flares when they occur, reduce organ damage and other problems. Treatments may include drugs to minimize swelling and pain, Prevent or decrease flares, Help the immune system, lessen or avoid damage to joints, Balance the hormones. In addition to medications for lupus itself, sometimes other medications are needed for lupus problems, such as high cholesterol, high blood pressure, or infection.
So, now that you seemed to know what lupus is, how did it change my life?
I go in & out of the hospital. Lupus totally changed my life.
I’m a mother of three children and love to cook, love to swim, love to work, who loves outdoors and a businesswoman and lives a very active life and a very hands-on mother. But everything changed 20 years ago, when little by little, for no reason, I’ve been getting sick; I will wake up several consecutive mornings feeling so tired, and getting out of bed was just too impossible. Then I will go for checkups, and the doctors will find nothing wrong with me…I will have mouth ulcers all over my gums, palate, and cheeks for weeks, sometimes months, that I needed to go to the dentist for help. I would have severe rashes when I get exposed to sunlight, and my fingers and toes will get too painful and can hardly be moved. And I needed to stop cooking completely because I’d get sick and feel overly fatigued after I do all the time. I will have severe headaches that I require to be hospitalized because I would lose control of my gut due to severe pain.
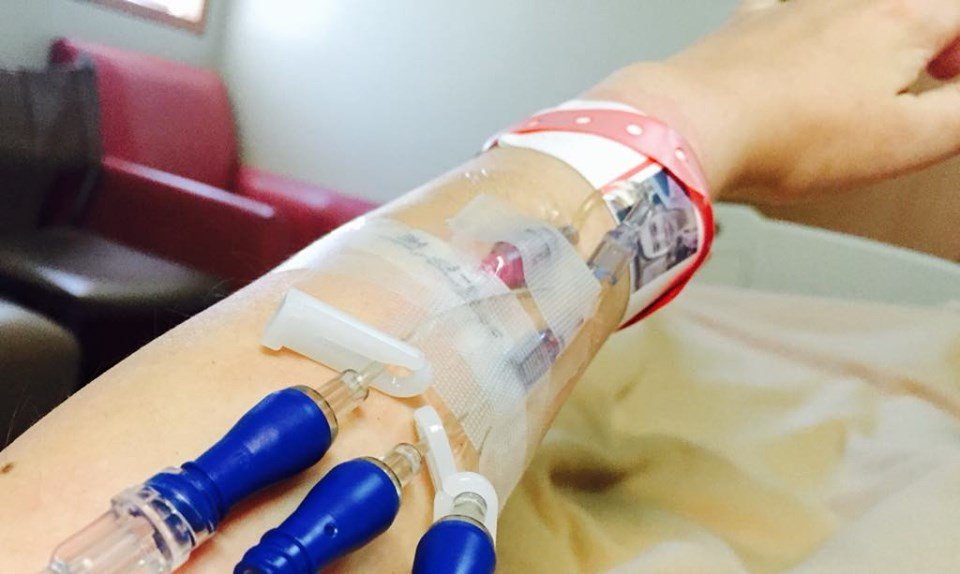
During my confinements in the hospital, I will usually need to have several IVs.
My family seemed to find it too impossible to be happening. My Ex-husband finds it so hard to believe and that it is real. Thus, I got depressed. Because my life just turned 360 degrees and I lost what I seemed to have, nobody appears to understand and believe how really I’m feeling. And my body and I really are feeling so weak, and it made me feel so alone. And I go in and out of the hospital more frequently. And my depression became a full-blown clinical depression.
Series of the test were made, such as Antinuclear antibody: Positive ANA antibody testing My life seemed to be turning upside down, and I don’t know why.
Then I got dengue! I got a high fever, believed it or not, my fingers and toes were so swollen and turned out to be like “jumbo hot dogs,” and they were so stiffed and too painful to move, and it was so impossible to bend. During this time, many tests were made, and finally, a real diagnosis came out… besides dengue, I was told to have – LUPUS or Systemic lupus erythematosus (SLE). Everything was explained, and it enlightened me up.
What do I do?
I must take an active role in my treatment. One key to living with lupus is to know about the disease and its impact. Being able to spot the warning signs helps me prevent the flare or make the symptoms less severe. Many people with lupus have certain symptoms just before a flare, such as: Feeling more tired, pain, rash, fever, stomach ache, headache, dizziness. I should see my doctor often, even when symptoms are not severe. These visits will help me and my doctor look for changes in symptoms to predict and prevent flares. Change the treatment plan as needed, Detect side effects of treatment. Typically, when the disease flares up (relapses) and symptoms become worse for a few weeks, sometimes longer. These relapses tend to alternate with times when symptoms settle down (remission). The reason why symptoms flare up or settle down is not yet fully understood.
It is also important to find ways to cope with the stress of having lupus. A good support system can also help. A support system may include family, friends. I have my parents, brothers and sister and family, kids, great friends from the church, and my BFF. Not everyone can accept and understand your situation and can live with you. Beware of them because since you will have many ups and downs during “flare-up times,” they will make your life more miserable and flare you up more. If they don’t believe you are sick, it is hard to get better and be well. They must know and understand what you’re going through.

Visiting during one of my confinements
Diagnosing lupus is difficult because signs and symptoms vary considerably from person to person. Signs and symptoms of lupus may vary over time and overlap with those of many other disorders. No one test can diagnose lupus. The combination of blood and urine tests, signs and symptoms, and physical examination findings leads to the diagnosis. It took me years.

“Bimbi and Friends”
From left: KC, Ping, JM, Barbie, Jackie. Center: I and
Fr. Clarence Canafe, LRMS.
Treatment for lupus depends on your signs and symptoms. Determining whether your signs and symptoms should be treated and what medications to use requires a careful discussion of the benefits and risks with your doctor. As your signs and symptoms flare and subside, you and your doctor may find that you’ll need to change medications or dosages. The medications most commonly used to control lupus include:
Nonsteroidal anti-inflammatory drugs (NSAIDs). Antimalarial drugs. Corticosteroids. Immunosuppressant
These are some additional facts about lupus that you should know:
· Lupus is not contagious, not even through sexual contact. You cannot “catch” lupus from someone or “give” lupus to someone.
· Lupus is not like or related to cancer. Cancer is a condition of malignant, abnormal tissues that grow rapidly and spread into surrounding tissues. Lupus is an autoimmune disease, as described above.
· Lupus is not like or related to HIV (Human Immune Deficiency Virus) or AIDS (Acquired Immune Deficiency Syndrome). With HIV or AIDS, the immune system is interactive; in lupus, the immune system is overactive.
· Lupus can range from mild to life-threatening and should always be treated by a doctor.

Whenever I don’t have flares, I maintain an active life. Who can tell I have Lupus?
Learning more about lupus is very important. Patients like me are important to be well informed and involved in their own care to have less pain make fewer visits to the doctor, feel better about ourselves, and remain more active.
Whenever I don’t have flares, I maintain an active life. Who can tell I have Lupus?
Sunscreen is a must! With or without the sun!
Important Tips: Avoid Stress. No Sunlight. Avoid being exposed to Extreme Heat and Extreme Cold. Don’t get infections by any means, and don’t overdo yourself! In-short, no-over fatigues!!!
 Copyright secured by Digiprove © 2020-2021 meline Ngo
Copyright secured by Digiprove © 2020-2021 meline Ngo

Hi everyone, it’s my first pay a quick visit atthis web page, and article is in fact fruitful for me, keep up posting these posts.
I needed to thank you for this great read!! I definitely enjoyed every little bit of it. I have you book-marked to check out new things you post…
amazing
I am using the theme called hueman pro. Hoping the same will suit you.
I checked your site and seems very good to me. Very slick. Doesn’t seem slow to me. But maybe your pictures are are too heavy. Try to use a smaller file.
Be well. Take care too.
Long time supporter, and thought I’d drop a comment.
Your wordpress site is very sleek – hope you don’t
mind me asking what theme you’re using? (and don’t mind
if I steal it? :P)
I just launched my site –also built in wordpress like yours– but the theme slows (!) the site down quite a bit.
In case you have a minute, you can find it by searching for “royal cbd” on Google (would appreciate any feedback) – it’s still in the
works.
Keep up the good work– and hope you all take care of yourself during the coronavirus scare!